Clubfoot is a congenital disorder that occurs in 1 out of 1,000 births per year. In newborns, the condition presents as the foot appearing as if it was rotated incorrectly at the ankle*. Several different factors cause clubfoot. Normally, clubfoot occurs due to genetics; however, some environmental factors are a possibility as well. Breech presentation and the position of the baby in a womb can cause clubfoot, as well as certain connective tissue disorders. This abnormality is often noticed during an ultrasound of the pregnancy at the 20th week.
A common treatment of clubfoot is reshaping. This is suggested to be done shortly after a child is born. The foot or feet are put into place and then casted on the legs* for stability. Required check-ups occur once a week to stretch and recast the feet. This process is done for about 5-10 weeks. Afterwards, one more cast is placed on for 3 weeks. Once positioned correctly, a child needs to wear a brace day and night for 3 months. For the next 3 years, while sleeping, the brace must be worn. These steps are taken to prevent the feet from reverting back to its misshapen position.
While this non-surgical approach has been proven very successful, severe cases of clubfoot may require surgery. Clubfoot surgery is usually performed after nine months of age. If surgery is performed, corrective shoes or a brace must be worn for up to a year afterwards as a supplemental measure. Secondary or repeat surgeries may also be needed to correct scar tissue damage as the child grows. In rarer cases, a surgical procedure may be needed as an adult.
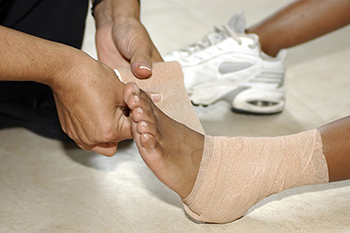
One of the most common causes of pain felt in the ankle region is a sprain. When ligaments in the ankle are torn or overstretched, an ankle sprain is likely to occur. There are three types of sprains that may develop: mild, moderate, and severe. In the case of a mild ankle sprain, the ankle is stable. The ligaments, however, are stretched. A moderate sprain consists of one or more ligaments being partially torn, and there’s limited movement. Severe ankle sprains include one or more torn ligaments, the ankle being unstable, and an inability to move the foot.
Ankle sprains are a common occurrence for those who are particularly active in sports. Volleyball, basketball, and soccer are just a few of the types of sports that are prone to producing ankle injuries, including ankle sprains. Many athletes have found that compressing the ankle by wrapping it in bandages is an effective method for helping to prevent injury. Exercising using a balance board has also been found useful for strengthening the ankle and increasing its stability.
If you’re experiencing ankle pain and believe you might have a sprain, it’s highly recommended that you consult with a podiatrist for a proper diagnosis and advised treatment plan.
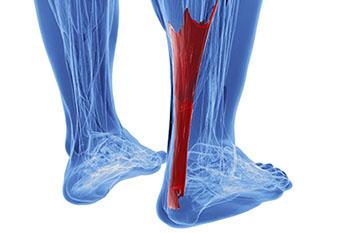
A condition that often results in serious heel pain is known as Achilles tendonitis. This condition may form when the Achilles tendon is damaged as a result of overuse. This particular injury can be very serious, as the Achilles tendon’s main function is to connect the lower half of the calf muscles to the heel bone. If this tendon becomes damaged, it may result in difficulty walking and completing everyday tasks, as well as cause extreme discomfort and pain.
It’s more common for athletes to experience Achilles tendon injuries, as they’re more likely to be participating in activities that would call for repetitive movement, such as running or jogging. This kind of repetitive movement over time is likely to cause stress on the tendon. When athletes abruptly increase their performance level without properly training or warming up their bodies, they may also injure the Achilles tendon, which may lead to inflexibility in the calf muscles.
In order to prevent this kind of injury, it’s suggested to perform stretches—particularly focused on the calf region—about one to three times a day to keep the area flexible. Focusing on building strength in your calves is also advised. If you believe you’ve injured your Achilles tendon, there are some actions you can take to help alleviate the discomfort. Icing and massaging the affected area may help to calm the pain, as well as practicing light stretches.
If you’re having difficulty walking or icing the area does not alleviate the pain, it’s highly advised that you speak with a podiatrist for professional care and an advised treatment plan.
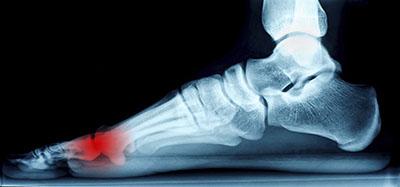
The pain caused by Morton’s neuroma is typically experienced at the ball of the foot. Many have described the sensation as feeling like they have a pebble stuck in their shoe. Because of this, those with the condition may find walking to be more difficult and uncomfortable. They may also experience a numbing or burning sensation in the foot. One of the most common factors that influence the development of Morton’s neuroma is improper footwear. Those who generally wear tightly fitted shoes or shoes with higher heels are more at risk at getting Morton’s neuroma. Having a foot abnormality may also increase the risk of getting this condition, as it may cause instability, thus adding more pressure onto the nerves of the foot. Certain foot conditions such as bunions, hammertoes, and flat flat feet have also been known to lead to Morton’s neuroma if not treated promptly.
Athletes have a tendency of getting Morton’s neuroma due to repetitive motions and pressure placed on the ball of the foot while running or jumping. Morton’s neuroma may also develop as a result of an injury to the foot.
To learn more about Morton’s neuroma and treatments that work best for your case, consult with your podiatrist.
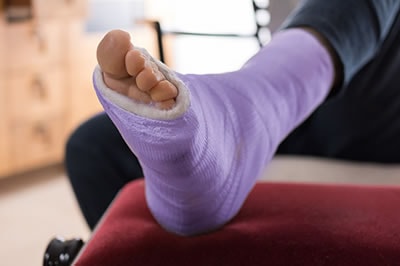 Stress fractures are small breaks in the bone that are caused by repetitive stress. They typically occur due to overuse, forcing the bones of the foot to continually absorb the full impact of each step someone takes. Stress fractures can also be caused by abnormal foot structure, osteoporosis, bone deformities, or wearing improper footwear during exercise.
Stress fractures are small breaks in the bone that are caused by repetitive stress. They typically occur due to overuse, forcing the bones of the foot to continually absorb the full impact of each step someone takes. Stress fractures can also be caused by abnormal foot structure, osteoporosis, bone deformities, or wearing improper footwear during exercise.
Stress fractures are common for individuals whose daily activities cause high levels of impact on their Feet. Individuals who run, play tennis or basketball, or practice gymnastics tend to experience these fractures more frequently. Anyone is susceptible to this problem, though. Individuals who are normally sedentary and suddenly begin an intense, high impact workout may sustain stress fractures. This is because their muscles are not yet strong enough to handle and cushion the intensity of their activity. Osteoporosis may also cause someone to get stress fractures, because the disease weakens an afflicted person's bones and makes it easier for them to break down.
Pain from stress fractures typically occurs in the general area of the fracture. Pain can also manifest as “pinpoint pain” or pain that is felt when the site of the injury is touched, and can be accompanied by swelling. It may occur during or after activity, and it may disappear while resting and return when standing or moving. Engaging in any kind of activity, high impact or otherwise, will aggravate the pain. If the intensity of the activity increases before the stress fracture has properly healed, it can cause a full fracture.
Treatment can vary depending on the individual and the degree of injury. The primary way to treat a stress fracture is to rest the hurt foot. Some fractures will heal quickly with only a little bit of rest, while others may require a long rest period and the use of crutches, immobilization, or physical therapy. Under certain circumstances, surgery may be required to install support pins around the fracture to assist in healing.
If you are undergoing a new exercise regimen in running or some other kind of high impact activity, set incremental goals on a weekly basis so you can build up muscle strength. Make sure to wear supportive shoes to better protect you feet.
If you begin to experience any symptoms of stress fractures, you should stop exercising and rest. If the symptoms persist, consult with your podiatrist. Remembering these tips can help you prevent stress fractures to your foot, and allow you to continue living normally.
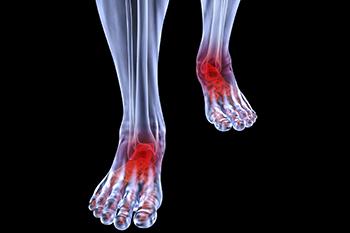 Although rheumatoid arthritis attacks multiple bones and joints throughout the entire body, ninety percent of people who actually develop this condition usually do so in the foot area. Those who develop this kind of arthritis in the feet usually develop symptoms around the toes and forefeet first, before anywhere else. Rheumatoid arthritis appears to have a genetic component. If it runs in the family, then you will be more likely to develop it as well.
Although rheumatoid arthritis attacks multiple bones and joints throughout the entire body, ninety percent of people who actually develop this condition usually do so in the foot area. Those who develop this kind of arthritis in the feet usually develop symptoms around the toes and forefeet first, before anywhere else. Rheumatoid arthritis appears to have a genetic component. If it runs in the family, then you will be more likely to develop it as well.
Rheumatoid arthritis is an autoimmune disorder in which the body’s own immune system attacks the lining of the membranes surrounding the joints. This causes inflammation of the membrane lining, and the gradual destruction of the joint’s cartilage and even bone.
Some of the most common symptoms that are associated with RA include pain and swelling of the feet. Stiffness in the feet is also another common symptom that people experience. Those who have RA in the feet usually feel the pain in the ball or sole of their feet. This can get to be very painful at times. A person's joints can even shift and become deformed after a period of time.
In order to properly diagnose RA in the feet it is usually necessary for a doctor or podiatrist to evaluate the area. Your doctor will also question you about your medical history, occupation, etc., to determine whether anything in your lifestyle may have triggered the condition. There are a number of tests that may be performed to help diagnose RA, such as a rheumatoid factor test. There is, however, no one single test that will tell you for sure if you have RA. There are different X-rays that can be taken as well to determine if a person has RA in their feet.
There is a range of treatment options for rheumatoid arthritis. Treatment of RA is usually a lifelong process that includes a variety of methods of treatment and therapy. Your doctor can prescribe special shoes that should help with arch support as well as heel support. A physical therapist can help those with this condition learn exercises which will keep their joints flexible. Surgery may be needed to correct some of the issues with the feet, such as bunions, and hammertoes. Fusion is usually the most successful surgical option for rheumatoid arthritis. However, people need to keep in mind that there are some risks associated with these surgeries.
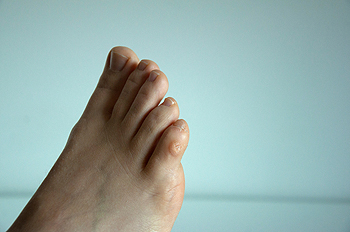 Corns are thickened areas on the skin’s surface, to the point of being irritating and sometimes painful. Commonly found on the feet, corns are circular or cone-shaped. They develop where there are areas of pressure or friction, such as on the little toe when it rubs up against shoes, or on the ball of your foot. The official medical term for corns is Helomas.
Corns are thickened areas on the skin’s surface, to the point of being irritating and sometimes painful. Commonly found on the feet, corns are circular or cone-shaped. They develop where there are areas of pressure or friction, such as on the little toe when it rubs up against shoes, or on the ball of your foot. The official medical term for corns is Helomas.
Corns are often confused with a callus, but there is a difference between them. Corns can be raised bumps that are painful to the touch. They consist of a rough, thick area of skin that may be dry or waxy. Corns tend to be surrounded by skin that is inflamed, and are usually much smaller than calluses.
Removing the dead skin that has built up is the key in treating corns. Salicylic acid medication is most common in accomplishing this. The acid works by dissolving keratin, which is the protein that makes up the majority of corns. You can purchase salicylic acid over-the-counter in products such as wart removers. It comes in a variety of forms such as medicated pads, drops, or creams. However, people who are diabetic should not use salicylic acid, but should instead consult their doctor immediately.
According to the product directions, applying the medication directly onto the corn will treat it. The top layer of the corn will begin to turn white after use. When that occurs, the layers of skin can then be peeled away, making the corn smaller. Shaving off corns with razors or other pedicure equipment is never a good idea. This can lead to infection. If your corn gets infected, and is not treated immediately, a visit to the doctor will be necessary.
Another way to treat corns and help prevent their return is by using orthotic inserts, fitted by a podiatrist. Inserts fit right into your shoes and adjusts the way your foot fits into your shoes. This fixes the way you walk. This will lower your chances of getting corns, and eliminate current corns by reducing rubbing from friction. Surgery is rarely used to treat corns, but does occur on occasion. Surgery actually deals with the underlying issue that causes corns. During surgery, the bone is shaved and any abnormalities are corrected, thus reducing the amount of friction that occurs during walking.
To prevent corns, the first step is reducing friction. Always wear shoes that fit well and don’t rub your feet. Pads can be purchased if you notice rubbing developing. These pads can be purchased over-the-counter, and can be simply placed on the irritated area. Wearing cushioned insoles in your shoes can always reduce the friction, and making sure to wear well-fitting shoes. This will ensure that your foot is not being squeezed awkwardly, and prevent corns from forming in the first place.
 The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
 Clubfoot is a congenital disorder that occurs in 1 out of 1,000 births per year. A clubfoot looks as though it was rotated incorrectly at the ankle*. Several different factors cause clubfoot. Normally, clubfoot occurs due to genetics; however, some environmental factors are a possibility as well. Breech presentation and the position of the baby in a womb can cause clubfoot, as well as certain connective tissue disorders. This abnormality is often noticed during an ultrasound of the pregnancy at the 20th week.
Clubfoot is a congenital disorder that occurs in 1 out of 1,000 births per year. A clubfoot looks as though it was rotated incorrectly at the ankle*. Several different factors cause clubfoot. Normally, clubfoot occurs due to genetics; however, some environmental factors are a possibility as well. Breech presentation and the position of the baby in a womb can cause clubfoot, as well as certain connective tissue disorders. This abnormality is often noticed during an ultrasound of the pregnancy at the 20th week.
A common treatment of clubfoot is reshaping. This is suggested to be done shortly after a child is born. The foot or feet are put into place and then casted on the legs* for stability. Required check-ups occur once a week to stretch and recast the feet. This process is done for about 5-10 weeks. Afterwards, one more cast is placed on for 3 weeks. Once positioned correctly, a child needs to wear a brace day and night for 3 months. For the next 3 years, while sleeping, the brace must be worn. These steps are taken to prevent the feet from reverting back to its misshapen position.
While this non-surgical approach has proven very successful, severe cases of clubfoot may require surgery. Clubfoot surgery is usually performed after nine months of age. If surgery is performed, corrective shoes or a brace must be worn for up to a year afterwards as a supplemental measure. Secondary or repeat surgeries may also be needed to correct scar tissue damage as the child grows. In rarer cases, a surgical procedure may be needed as an adult.
 Sesamoiditis is a condition that affects the joint that is just behind the big toe in the area known as the ball of the foot. It is most common in younger people and people who have just begun an exercise program. Since the sesamoid bones are like a pulley controlling the big toe, they can rub against each other and cause a gradual onset of pain. Pain may also be caused by the inflammation of tendons surrounding the bones. If ignored, sesamoiditis can lead to other, more serious problems such as severe irritation and fractures of the bones.
Sesamoiditis is a condition that affects the joint that is just behind the big toe in the area known as the ball of the foot. It is most common in younger people and people who have just begun an exercise program. Since the sesamoid bones are like a pulley controlling the big toe, they can rub against each other and cause a gradual onset of pain. Pain may also be caused by the inflammation of tendons surrounding the bones. If ignored, sesamoiditis can lead to other, more serious problems such as severe irritation and fractures of the bones.
The cause of sesamoiditis is sudden increase in activity. The ball of your foot acts as a springboard to help you lift off when you are jogging or running. Sudden increase in the use of these bones or the tendon that controls them can cause irritation. The tendon then begins to develop inflammation and the joint begins to swell. People with smaller, bonier feet or those with a high arch are typically more susceptible to this condition.
Sesamoiditis is fairly simple to diagnose since the symptoms have a gradual onset rather than a sudden impact. The symptoms begin with slight irritation around the joint shortly after the increase in activity. The discomfort eventually turns to pain with light swelling and possible redness. Although redness or bruising is rare either may occur. After each session of exercising, the aggravated joint becomes more irritated and can exacerbate into intense throbbing.
Treatment for sesamoiditis can vary depending on the severity of the condition. However, treatment for sesamoiditis is almost always approached in a noninvasive way. For a case that is just beginning, the doctor may recommend a very strict rest period that will limit the activity allowed on the joint. If you must be active, a recommendation for a modified shoe or insole along with bandaging and immobilizing the big toe will be made to ensure that pressure is not placed on the joint. For severe cases, it is typically recommended that the joint and the big toe be completely immobilized to allow adequate time to heal. Ice and an over-the-counter anti-inflammatory may can help with the pain and discomfort while you are at rest.
When you return to your regular exercise activities, it is recommended that you use an insole that will allow even distribution of impact to your entire foot, rather than just the ball of your foot. This will prevent further aggravation of the condition.
This condition is a lasting pain on the outer side of the ankle that often develops after an injury such as a sprain or fracture of the ankle.
The most common cause for chronic ankle pain is a failure of the ankle to heal properly after an injury. If the pain develops after a sprain, the affected ligament may remain weak after healing, causing instability and the chance for further injury.
Nerves and tendons may also be injured in the sprain, and scar tissue may develop, placing pressure on structures in the ankle.
The most common symptom is lasting pain on the outer side of the ankle, particularly when walking or when participating in sports or strenuous exercise. Other symptoms include difficulty walking, instability, swelling, stiffness and tenderness.
Treatment options include anti-inflammatory medication, physical therapy, use of a cast, splint or brace, and rest. If the pain continues for a considerable time after treatment, surgery may be required.
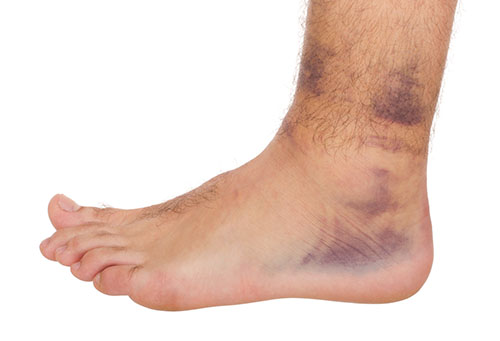 Although ankle sprains may not be as serious as a broken ankle, they should be given immediate attention and care. An ankle sprain can lead to a significant amount of pain, as well as limited mobility. They are often characterized by the swelling and discoloration of the skin. This occurs when the ligaments are stretched beyond their limits. The simple act of walking can sometimes cause a sprain, which makes ankle sprains a very common injury that can happen to anyone. They occur when the ankle twists in an awkward way or rolls over itself, causing a pop or snap in the tendons around the ankle. Some people are more at risk than others. These include athletes who continually push their bodies to the limits and also people who have previously suffered accidents to the feet, ankles, or lower legs.
Although ankle sprains may not be as serious as a broken ankle, they should be given immediate attention and care. An ankle sprain can lead to a significant amount of pain, as well as limited mobility. They are often characterized by the swelling and discoloration of the skin. This occurs when the ligaments are stretched beyond their limits. The simple act of walking can sometimes cause a sprain, which makes ankle sprains a very common injury that can happen to anyone. They occur when the ankle twists in an awkward way or rolls over itself, causing a pop or snap in the tendons around the ankle. Some people are more at risk than others. These include athletes who continually push their bodies to the limits and also people who have previously suffered accidents to the feet, ankles, or lower legs.
Most of the time, an ankle sprain is not severe enough for hospital attention. There are many at-home treatment options available, including propping the leg up above your head to reduce blood flow and inflammation, applying ice packs to the affected area as needed, taking over the counter pain relievers and anti-inflammatory medication, using an ACE bandage to wrap and support the injured ankle, and most importantly, remaining off your feet until the ankle has fully healed.
Despite this, an ankle sprain can turn into a severe injury that might require hospitalization. If the ankle ligaments or muscles are damaged from a tear or rip, that is one sign that the sprain is severe enough for hospital attention and possibly for surgery. Even after the surgery, the recovery process can be long. You may need to have rehabilitation sessions administered by your podiatrist to get your ankle back to full health.
The severity of your sprain might become apparent if you are unable to stand or walk, consistent pain is occurring over a prolonged period of time, swelling is much more severe than initially present, or if you start to experience tingling or numbness. These signs may indicate that your ankle sprain might actually be a broken ankle, an injury that requires immediate medical attention.
Although they are not completely avoidable, ankle sprains can be curbed with some preventative treatment measures. These include wearing appropriate fitting shoes that not only provide a comfortable fit, but also ankle support. It is also recommended to stretch before doing any kind of physical activity, as this will help lower your body’s chance for an injury.
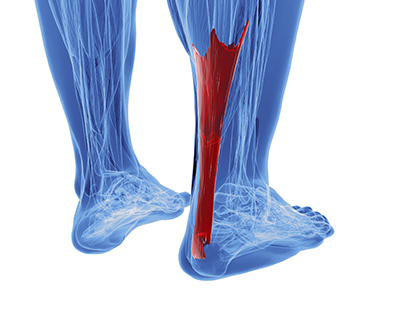 The Achilles tendon is the strongest tendon in the human body. Its purpose is to connect the lower leg muscles and calf to the heel of the foot. This tendon is responsible for facilitating all types of movement, like walking and running. This tendon provides an enormous amount of mobility for the body. Any injuries inflicted to this tissue should be immediately brought up with a physician to prevent further damage.
The Achilles tendon is the strongest tendon in the human body. Its purpose is to connect the lower leg muscles and calf to the heel of the foot. This tendon is responsible for facilitating all types of movement, like walking and running. This tendon provides an enormous amount of mobility for the body. Any injuries inflicted to this tissue should be immediately brought up with a physician to prevent further damage.
The most common injuries that can trouble the Achilles tendon are tendon ruptures and Achilles tendinitis. Achilles tendinitis is the milder of the two injuries. It can be recognized by the following symptoms: inflammation, dull to severe pain, an increased flow of blood to the tendon, thickening of the tendon, and slower movement time. Tendinitis can be treated via several methods and is often diagnosed by an MRI.
An Achilles tendon rupture is trickier to heal, and is by far the most painful injury. It is caused by the tendon ripping or completely snapping. The results are immediate and absolutely devastating, and will render the patient immobile. If a rupture or tear occurs, operative and non-operative methods are available. Once the treatment begins, depending on the severity of the injury, recovery time for these types of issues can take up to a year.
Simple preventative measures can be taken as a means to avoid both injuries. Prior to any movement, taking a few minutes to stretch out the tendon is a great way to stimulate the tissue. Calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses are all suggested ways to help strengthen the lower legs and promote Achilles tendon health.
Many problems arise among athletes and people who overexert themselves while exercising. Problems can also happen among those who do not properly warm up before beginning an activity. Proper, comfortable shoes that fit correctly can also decrease tendon injuries. Some professionals also suggest that when exercising, you should make sure that the floor you are on is cushioned or has a mat. This will relieve pressure on the heels. A healthy diet will also increase tendon health.
It is very important to seek out a podiatrist if you believe you have an injury in the Achilles region. Further damage could result in severe complications that would make being mobile difficult, if not impossible.
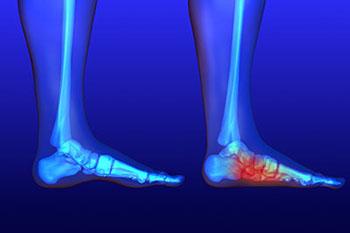 Flatfoot is a foot condition in which the arch of the foot has either partially or totally dropped or has never developed. While it is common in babies and small children, it can become a problem for them in adulthood if the arch never forms. For adults, the development of flat feet can be brought upon by injury, as a result of pregnancy due to increased elasticity, or obesity. Those who have health concerns such as rheumatoid arthritis or diabetes may also be at greater risk for developing the condition.
Flatfoot is a foot condition in which the arch of the foot has either partially or totally dropped or has never developed. While it is common in babies and small children, it can become a problem for them in adulthood if the arch never forms. For adults, the development of flat feet can be brought upon by injury, as a result of pregnancy due to increased elasticity, or obesity. Those who have health concerns such as rheumatoid arthritis or diabetes may also be at greater risk for developing the condition.
If you suspect that you have flat feet, it is best to consult your podiatrist. Your foot doctor will examine the suspected foot and observe how it looks while you sit and stand. He or she may take an X-ray to determine how serious the condition is. Some common signs of flatfoot include toe drift, in which the toes and front part of the foot point outward, a short Achilles tendon, and a heel that tilts outwardly while the ankle* tilts inward.
Once flatfoot has been diagnosed, your podiatrist may suggest one of several treatment options. Flat feet can be rigid, in which the feet appear to have no arch even when the person is not standing; or flexible, in which the person appears to have an arch while not standing, but once standing the arch disappears. Those with flexible flatfoot may be told to reduce any activities that cause pain and to avoid extended periods of walking or standing. Another suggestion may be weight loss, as excessive weight may be placing pressure on the arches
In few cases, if the condition is severe and all other methods have been exhausted surgery may be required. This is normally avoided, however, due to a lengthy recovery time and high cost.
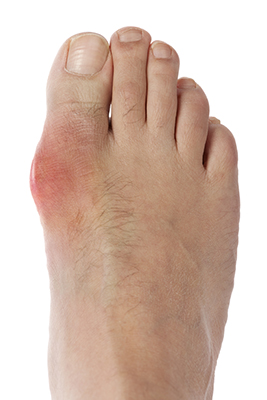 Gout, typically found in diabetic patients, is an unusually painful form of arthritis caused by elevated levels of uric acid in the bloodstream. The condition typically strikes the big joint on the big toe. It has also been known to strike the knees, elbows, fingers, ankles and wrists—generally anywhere that has a functioning, moving joint. The high level of uric acid in a person’s bloodstream creates the condition known as hyperuricema—the main cause of gout. Genetic predisposition occurs in nine out of ten sufferers. The children of parents who suffer gout will have a two in ten chance of developing the condition as well.
Gout, typically found in diabetic patients, is an unusually painful form of arthritis caused by elevated levels of uric acid in the bloodstream. The condition typically strikes the big joint on the big toe. It has also been known to strike the knees, elbows, fingers, ankles and wrists—generally anywhere that has a functioning, moving joint. The high level of uric acid in a person’s bloodstream creates the condition known as hyperuricema—the main cause of gout. Genetic predisposition occurs in nine out of ten sufferers. The children of parents who suffer gout will have a two in ten chance of developing the condition as well.
This form of arthritis, being particularly painful, is the leftover uric acid crystallizing in the blood stream. The crystallized uric acid then travels to the space between joints where they rub, causing friction when the patient moves. Symptoms include: pain, redness, swelling, and inflammation. Additional side effects may include fatigue and fever, although reports of these effects are very rare. Some patients have reported that pain may intensify when the temperature drops, such as when you sleep. Most cases of gout are easily diagnosed by a podiatrist’s assessment of the various symptoms. Defined tests can also be performed. A blood test to detect elevated levels of uric acid is often used as well as an x-ray to diagnose visible and chronic gout.
Treatment for gout simply means eliminating symptoms. Non-steroid anti-inflammatory drugs or NSAIDs (Colchicine and other corticosteroid drugs, etc.) will quell the redness, the swelling, and the inflammation. However, managing your diet, lifestyle changes, and using preventative drugs are all helpful toward fully combating the most severe cases.
Those that lead an inactive lifestyle are at a higher risk for gout. Any amount of exercise decreases the probability of repeat encounters with the condition. Reducing your consumption of red meat, sea food, and fructose-sweetened drinks also reduces the likelihood of chronic gout as well.
Ingesting Vitamin C, coffee, and particular dairy products can help with maintaining a healthy lifestyle. There are new drugs out on the market that inhibit the body’s production of uric acid-producing enzymes. However, reducing or eliminating your overall levels of uric acid is the best remedy to ensuring you lead a gout-free life.
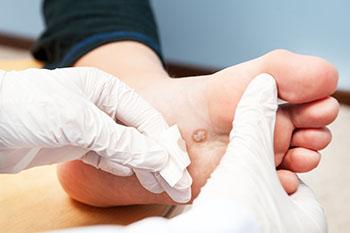 Plantar warts are warts that are only found on the feet, hence the term “plantar”, which means “relating to the foot.” They are caused by the human papillomavirus, or HPV, and occur when this virus gets into open wounds on the feet. The warts themselves are hard bumps on the foot. They are easily recognizable, mostly found on the heels or ball of the foot. Plantar warts are non-malignant, but they can cause some pain, discomfort, and are often unsightly. Removing them is a common step toward treating them.
Plantar warts are warts that are only found on the feet, hence the term “plantar”, which means “relating to the foot.” They are caused by the human papillomavirus, or HPV, and occur when this virus gets into open wounds on the feet. The warts themselves are hard bumps on the foot. They are easily recognizable, mostly found on the heels or ball of the foot. Plantar warts are non-malignant, but they can cause some pain, discomfort, and are often unsightly. Removing them is a common step toward treating them.
Plantar warts can cause some pain while standing, sometimes felt as tenderness on the sole of your foot. Unless the wart has grown into the foot behind a callus, you will be able to see the fleshy wart. A podiatrist should only be consulted if there is an excessive amount of pain. Plantar warts are not cancerous or dangerous, but they can affect your walking and continually reappear. Anyone who suffers from diabetes or a compromised immune system disease should seek out care immediately.
Podiatrists are easily able to diagnose plantar warts. They usually scrape off a tiny bit of the rough skin to make tiny blood clots visible and examine the inside of warts. However, a biopsy can be done if the doctor is not able to diagnose them from simply looking at them. Although plantar warts usually do not require an excessive amount of treatment, there are ways to go about removing them. A common method is to freeze them off using liquid nitrogen, removing them using an electrical tool, or burning them off via laser treatment. For a less invasive treatment option, topical creams can be used through a doctor’s prescription. This treatment method takes more time, however. Keep the wart covered for protection in between daily treatments.
The best way to avoid developing plantar warts is to avoid walking barefoot in public places. Avoid this especially if you have open sores or cuts on your feet. It is also important to avoid direct contact with warts in general, as they are highly contagious.

Please feel free to browse our expanded Patient Education library using the topics listed below.

Corns
Diabetic Foot
Gout
Plantar Warts
Rheumatoid Arthritis of the foot
Stress Fractures of the foot
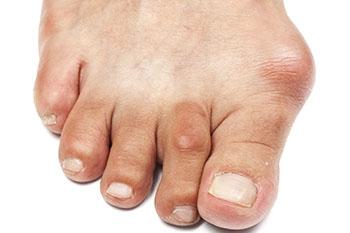 A bunion is an enlargement of the base joint of the toe that connects to the foot, often formed from a bony growth or a patch of swollen tissues.It is caused by the shifting of the big toe bone inward towards the other toes. This shift can cause a serious amount of pain and discomfort. The area around the big toe can become inflamed, red, and painful.
A bunion is an enlargement of the base joint of the toe that connects to the foot, often formed from a bony growth or a patch of swollen tissues.It is caused by the shifting of the big toe bone inward towards the other toes. This shift can cause a serious amount of pain and discomfort. The area around the big toe can become inflamed, red, and painful.
Bunions are most commonly formed in people who are already genetically predisposed to them or other kinds of bone displacements. However, even if you do not have a history of this in your family, you can still develop bunions if you are wearing improperly fitting shoes. This can happen as you try to cram your feet into high heels, or by running or walking in a way that causes too much stress on the feet. High heels are another major culprit in the formation of bunions. Not only do they push the big toe inward, but your body weight and center of gravity is shifted towards the edge of your feet and your toes, which can cause bone displacement.
Bunions are quickly and easily diagnosed by podiatrists. However, because of their nature, they can appear similar to arthritic conditions or gout. A blood test is sometimes required to fully diagnose a bunion. A full radiological or x-ray exam could also be done by a podiatrist to examine the bone structure of your feet. One thing that is looked for specifically is an enlargement of that base joint or evidence of the big toe bone being pushed inward.
One of the first things to do if you have bunions is to get a larger, wider shoe that can remove pressure from your toes. This usually means that high heels should be eliminated from use for a period of time to allow the bunion to heal. Eliminating the pressure placed on a bunion is often enough to eliminate the pain involved with them. However, pain can persist in some instances and anti-inflammatory drugs may be prescribed. If the pain is too severe, steroid injections near the bunion or even surgery may be required. Orthotics for shoes may also be prescribed which can alleviate the pain of bunions by removing pressure from them. However, these methods simply stop the pain of bunions but do not correct the problem at its source.
As previously mentioned, surgery may be an option to completely eliminate your bunions. Surgery is done to reposition the toe bones so that they no longer face inward. This can be done by removing a section of bone or by rearranging the ligaments and tendons in the toe to help them align properly. Even after the surgery, it may be necessary to wear protective shoes for a while to ensure that the bunions do not return.
Foot surgery may be performed depending on the severity of the injury. In any case, if you happen to develop a foot condition, it’s always advised you seek the counsel of a podiatrist for a proper diagnosis and advised treatment plan. If you notice an abnormal growth, a change in the appearance of your foot, discomfort while standing or walking, or general foot pain, it would be in your best interest to seek professional help, especially if surgery is the recommended treatment for your case.
Podiatrists perform foot surgery to treat a number of different conditions. These may include bunions, heel pain, flat feet, arthritis of the foot, sports injuries, hammertoes, ingrown toenails, complications due to diabetes, and fractures, to name a few. Again, the need for surgery is dependent upon the type of injury you are experiencing, as well as its severity. This also means that the recovery process for surgery will vary as well. With that being said, most podiatrists will recommend you get plenty of rest, stay off your feet, ice the affected area to reduce swelling, and elevate the affected area.
If you believe you have a foot injury that may require surgery, it’s highly recommended that you speak with a podiatrist as soon as possible to go over the best treatment option for your condition.

When it comes to receiving foot and ankle surgery, it’s typically a case by case situation. Some factors that play a role in whether or not you need surgery include the severity of your symptoms as well as your response to other conservative, noninvasive treatment methods.
There are a number of different foot and ankle conditions that may benefit from surgery as a treatment option. Bunions, hammertoe, metatarsal, ankle arthritis, Achilles tendon disorders, Morton’s neuroma, tibialis posterior disorder, and plantar fasciitis are all conditions that may require surgery as a treatment option, depending on their severity. Long-lasting pain relief is typically the biggest takeaway from having surgery performed to remedy your condition.
In order to best prepare for surgery, make sure you have a consultation with your podiatrist about your overall health, discuss any possible changes in medication, and ask any questions you may have about the procedure to go into the treatment with a clear head. In some cases, you may have to refrain from eating and drinking a few hours before the procedure, so make sure you understand what must be done on your end beforehand.
As for recovery, again, this will typically vary case by case and will be dependent on your condition and the type of surgery performed. Generally, it’s recommended that you get plenty of rest, ice the affected area, compress the wound to aid in further strain, and keep the area elevated to reduce any possible swelling. In some cases, your podiatrist may encourage you to use bandages, splints, surgical shoes, casts, crutches, orthotics, or a cane, depending on how much weight they believe your foot and ankle can bear.
If you’d like to determine whether surgery is the best option for you and your foot condition, consult with a podiatrist who will be able to give you a proper diagnosis and aid you with your decision.
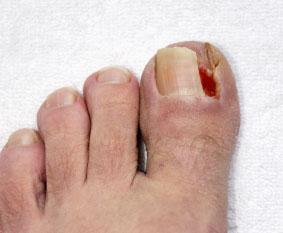
Signs that may indicate the formation of an ingrown toenail include redness, pain, swelling of the surrounding skin, possible bleeding or oozing of pus, and an overgrowth of the skin around the nail. The surrounding skin may also feel tender and become swollen or hardened. Most ingrown toenails are diagnosed by a simple physical exam; however, an x-ray may be required to show how deep the nail has grown into the skin of the toe.
Many factors influence the likelihood of developing an ingrown toenail. The most common way ingrown toenails are formed is due to an incorrect method in how the toenails are trimmed. If you cut your toenails too short or cut them at an angle, you’re putting yourself at risk of getting this condition. Another main factor that contributes to ingrown toenails is the choice of footwear. Those who commonly wear tightly fitted shoes, such as high heels, that do not give the toes enough room, put too much pressure on the big toes. This can create an ingrown toenail. To alleviate the pain, a small piece of cotton may be fitted underneath the nail. However, in more serious cases, total removal of the nail may be necessary.
For a proper diagnosis and advised treatment plan, we recommend you seek the care of a podiatrist as soon as you notice the warning signs of an ingrown toenail.
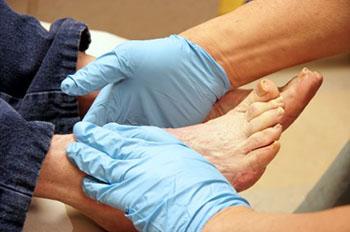
Diabetes can unfortunately cause many foot problems that often lead to a great deal of pain and discomfort. For example, poor circulation of the feet is often an issue among those with diabetes because it damages the nerves. When this occurs, it’s likely for one to develop peripheral neuropathy. Peripheral neuropathy can make it feel like you have pins and needles in your feet. Others who have experienced this condition have also recalled a burning, tingling, or numbing sensation.
Since nerves are often damaged due to diabetes, the issue of not feeling when a wound has developed can lead to serious complications. Minor cuts or scrapes on the foot may run the risk of getting infected if the feet are not checked daily for wounds. Diabetes may also reduce blood flow to the feet, which in turn can make it harder for wounds to heal. With that being said, it’s important you seek professional help for treating any foot ailments. To prevent yourself from running the risk of developing a serious foot condition, it’s recommended that you wash and dry your feet daily, cut your toenails carefully, keep your feet moisturized, check them regularly for any abnormalities, and keep your feet warm and dry.
For more advice on how to care for diabetic feet, we suggest you consult with a podiatrist for professional care and a recommended treatment plan for any existing conditions.
This condition is a bony enlargement on the back of the heel that can aggravate the retrocalcaneal bursa, a fluid-filled sac located on the back of the heel between the Achilles tendon and the calcaneus. The bursa can become inflamed and swollen, a condition called bursitis. Haglund's deformity most commonly affects young women.
Haglund's deformity commonly develops as a result of wearing shoes with rigid backs, such as pumps, which put pressure on the back of the heel.
Over time, this pressure can cause a bony bump to form on the calcaneus, and this bump digs into the surrounding soft tissue. The irritated bursa swells, and other tissues, including the Achilles tendon, may swell and thicken.
People who have certain anatomical structures, such as a prominent bump underneath the Achilles tendon, high arches, a tight Achilles tendon, or other factors have an increased susceptibility to this condition.
Symptoms include pain and a callus at the back of the heel. If bursitis develops, a large, swollen bump may form on the back of the heel.
Treatment options include wearing shoes with no backs or soft backs, heel pads or other orthotic devices, heel sleeves, ice, anti-inflammatory medications and physical therapy. In some cases, a cast or boot may be needed. In severe cases, surgery may be needed to remove the bony bump or alter the shape of the calcaneus.
© 2008 Swarm Interactive, Inc.
This condition is a break in the heel bone, called the calcaneus, which forms the back of the foot. This bone supports the foot and is important for normal walking.
Fractures of the heel bone most commonly occur from severe trauma to the foot, often from a motor vehicle accident or a fall. Small fractures can also occur in athletes who are required to place stress on the foot for long periods of time, such as long-distance runners. Some calcaneus fractures can be associated with other injuries to the bones of the thigh, leg, or even the spine.
Symptoms of a heel bone fracture can include pain and swelling in the back of the foot or on the bottom of the heel, inability to walk, and bruising. A severe fracture may break through the skin.
Treatment options include use of a cast, splint or brace, anti-inflammatory medication, cold compress, and therapy after the removal of a splint. In cases where the bones of the foot have moved out of alignment, surgery may be required.
© 2008 Swarm Interactive, Inc.
Heel pain is most commonly caused by repetitive stress. With that being said, it may be more common for athletes who perform repetitive movements to be afflicted with heel pain at some point during their activity. Heel pain can occur due to a number of different factors. These may include issues with having poor circulation, complications due to arthritis and diabetes, and poor form when running or exercising, as well as having poor posture.
There are a number of conditions that may also influence pain felt in the heel region. Tarsal tunnel syndrome is one example of a condition that affects the heel. This may occur when the nerve in the back of the foot becomes pinched, thus causing a numbing or tingling feeling as if the heel has pins and needles in them. Heel bursitis is another condition that commonly brings discomfort to the heel. This condition may arise when inflammation occurs at the back of the heel, often occurring due to landing awkwardly or wearing footwear that puts a good amount of pressure on the heel. As a result, the Achilles tendon may swell, causing the pain to increase throughout the day. Simple exercises focused on strengthening the heel and surrounding areas, as well as focused on building the flexibility of the foot, may help to prevent and treat heel pain.
For a proper diagnosis and advised professional treatment plan, we recommend that you consult with a podiatrist as soon as possible to avoid developing a serious condition.